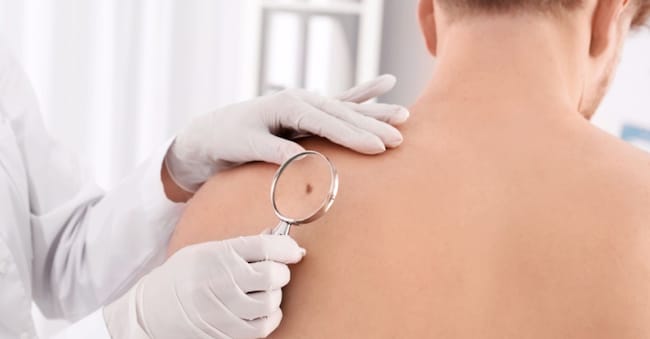
Skin cancer prevention: why it is essential
Skin cancer prevention is a key tool for reducing the risk of developing melanoma. Regular skin check-ups, combined with knowledge of one's own risk factors and observation of moles, allow early detection of any suspicious lesions and timely intervention.
We spoke about this with professor Franco Rongioletti, head of Clinical Dermatology at IRCCS Ospedale San Raffaele in Milan of Gruppo San Donato, a facility that since 2025 has been recognised as a Comprehensive Cancer Centre.
Dermatological examination and mole mapping: the differences
When it comes to skin cancer prevention, it is essential to distinguish between a dermatological examination and mole mapping.
"The dermatological examination is a clinical assessment carried out at a specific time: the dermatologist looks at the skin with the naked eye and with a dermatoscope to identify any suspicious lesions. It is a snapshot of the skin condition," explains Prof. Rongioletti. "
Nevus mapping, on the other hand, represents a more advanced level of control: it integrates the examination with photographic documentation of the entire body and the most significant nevi, creating a digital archive that allows comparisons over time. This dynamic approach is particularly effective in the prevention of melanoma'.
The ABCDE of moles for self-assessment
A simple but effective method for recognising suspicious lesions at an early stage is the ABCDE rule:
- A - Asymmetry: one half of the nevus does not correspond to the other; any changes in symmetry over time are relevant;
- B - Edges: irregular, jagged or poorly defined margins;
- C - Colour: presence of multiple colours or uneven shades;
- D - Size: diameter greater than 6 mm (although smaller lesions may be suspect);
- E - Evolution: changes over time (shape, colour, size or symptoms such as itching or bleeding).
In the presence of one or more of these signs, it is important to consult the dermatologist for a thorough evaluation.
The importance of monitoring over time
Mapping makes it possible to detect even minute changes in the shape of the mole, often imperceptible to the patient, and to make an early diagnosis, which is fundamental: intercepting the lesion in the early stages allows, in most cases, a complete healing. Monitoring over time is therefore central to the preventive strategy.
"The frequency of check-ups depends on the individual risk profile," explains the specialist. In the absence of predisposing factors, an annual visit is generally adequate. It is different in the case of subjects with numerous nevi, a light phototype, blond or red hair, light-coloured eyes, or with a history of intense exposure to ultraviolet rays or a personal or family history of melanoma; in these cases, the dermatologist may indicate more frequent check-ups, often every six months, and the systematic use of digital mapping for a more accurate follow-up".
How the examinations are carried out
After a complete assessment of the skin surface, the dermatologist uses the dermatoscope to analyse the more detailed structures of the nevi, improving the ability to distinguish benign from suspicious lesions.
Digital mapping is supplemented by the recording of high-resolution images, which are archived and compared at subsequent visits. This comparison over time significantly increases diagnostic accuracy and reduces the risk of underestimating evolving lesions.
Main Risk Factors
The main risk factors for melanoma include:
- exposure to ultraviolet rays, especially with sunburn in childhood or adolescence;
- presence of numerous nevi or atypical nevi;
- phenotypic features such as fair skin, fair hair and light-coloured eyes;
- use of tanning lamps: exposure to artificial UV, especially at a young age, significantly increases the risk.
A previous diagnosis of skin cancer or conditions of immunodepression also contribute to an increased risk.
The role of familiarity and genetics
The familiarity is of particular importance; having first-degree relatives with melanoma significantly increases an individual's risk and requires a more rigorous preventive approach. In such cases, check-ups should be started at an earlier age and maintained more regularly.
Alongside clinical factors, genetics also contribute to predisposition. "Mutations in genes such as CDKN2A and CDK4 are associated with an increased risk of developing melanoma," explains Rongioletti. In contexts of strong familiarity, the specialist can propose genetic tests to define the individual risk profile and plan personalised surveillance programmes.
"Integrating periodical dermatological check-ups with self-observation, through the ABCDE rule, and - when indicated - with digital mapping of nevi means adopting a truly effective strategy for skin protection," Rongioletti concludes.